Unlocking the Potential of Food Addiction Therapy with GLP-1
Food addiction is a complex and multifaceted issue that affects millions of people worldwide. While traditional treatments focus on diet and lifestyle changes, a new wave of research is exploring the possibility of using GLP-1 (Glucagon-like peptide-1) medications to treat food addiction. In this article, we'll delve into the world of GLP-1 and its potential role in food addiction therapy.
What is GLP-1 and How Does it Work?
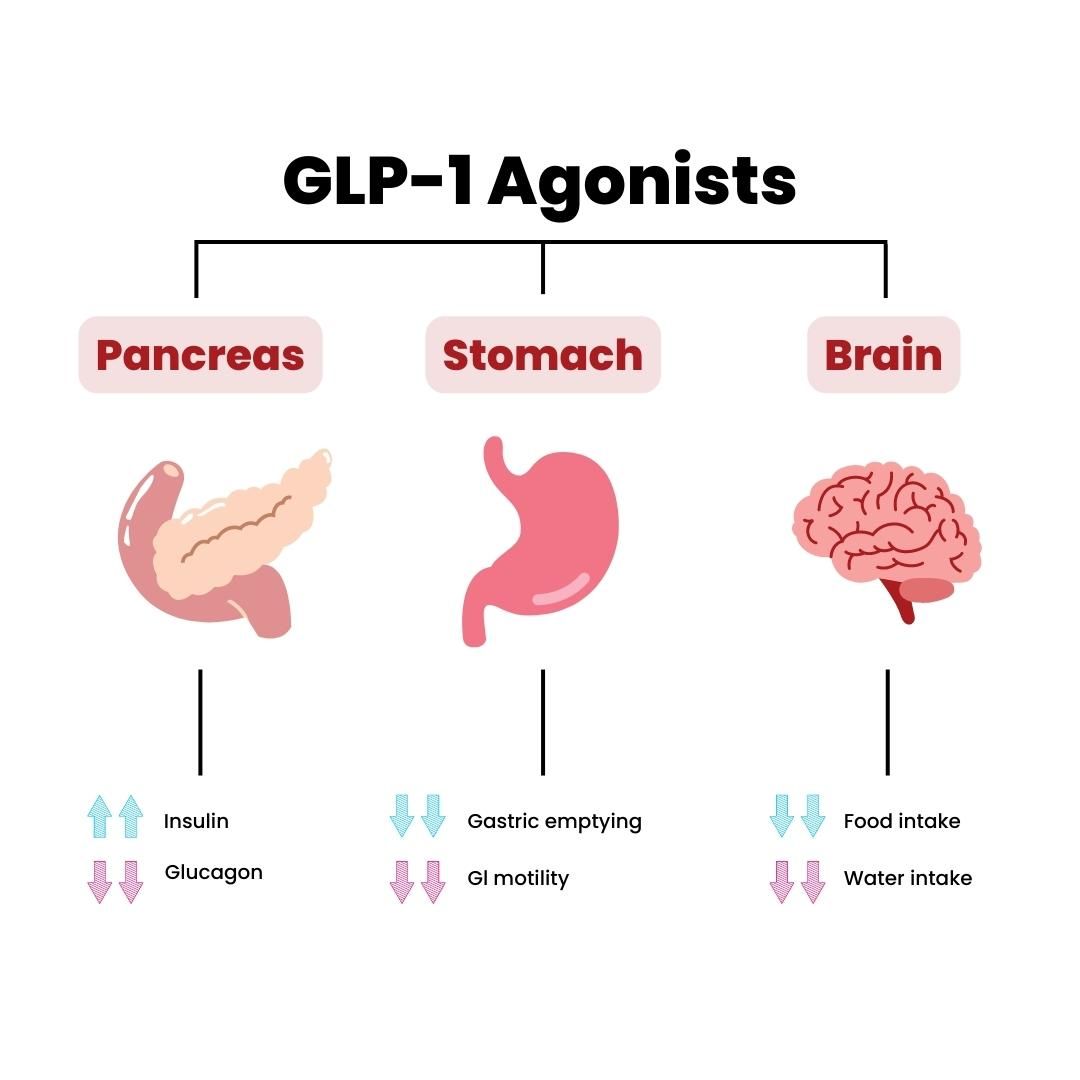
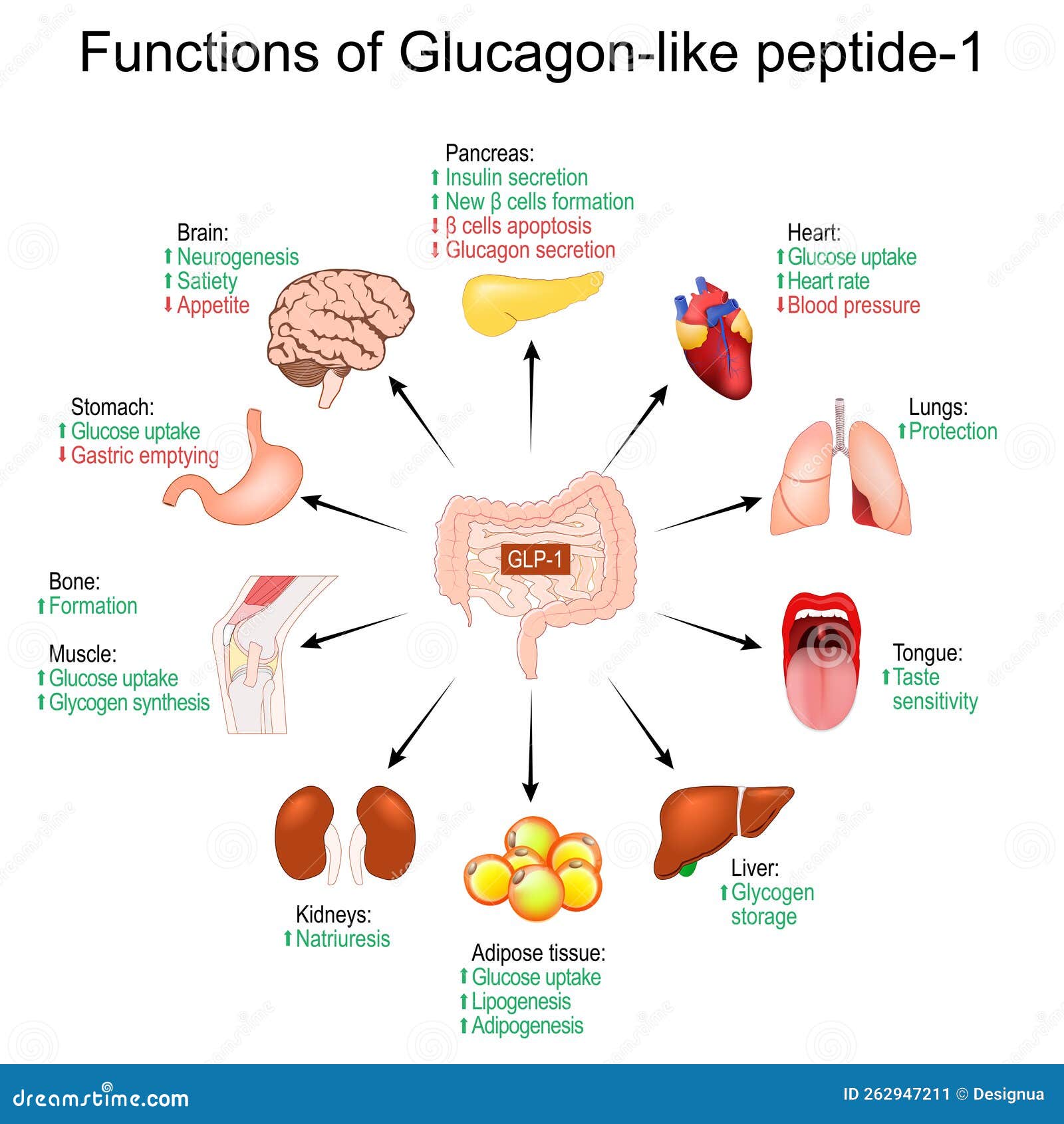
GLP-1 is a naturally occurring hormone involved in appetite regulation, digestion, and insulin release. Typically, GLP-1 medications have been used to treat type 2 diabetes and obesity by slowing gastric emptying, increasing satiety, reducing hunger, and food cravings. However, emerging evidence suggests that GLP-1 may also have a profound effect on the brain's reward system, making it a promising candidate for treating food addiction.
GLP-1 and Food Addiction: Breaking the Cycle

Food addiction is often characterized by compulsive eating, intense cravings, and loss of control. GLP-1, with its ability to regulate appetite and reduce cravings, may help individuals break the cycle of food addiction. By targeting the brain's dopamine reward system, GLP-1 could potentially reduce the emotional and psychological association with food, leading to a more balanced and sustainable relationship with eating.
From Weight Loss to Addiction Treatment: The Emerging Role of GLP-1
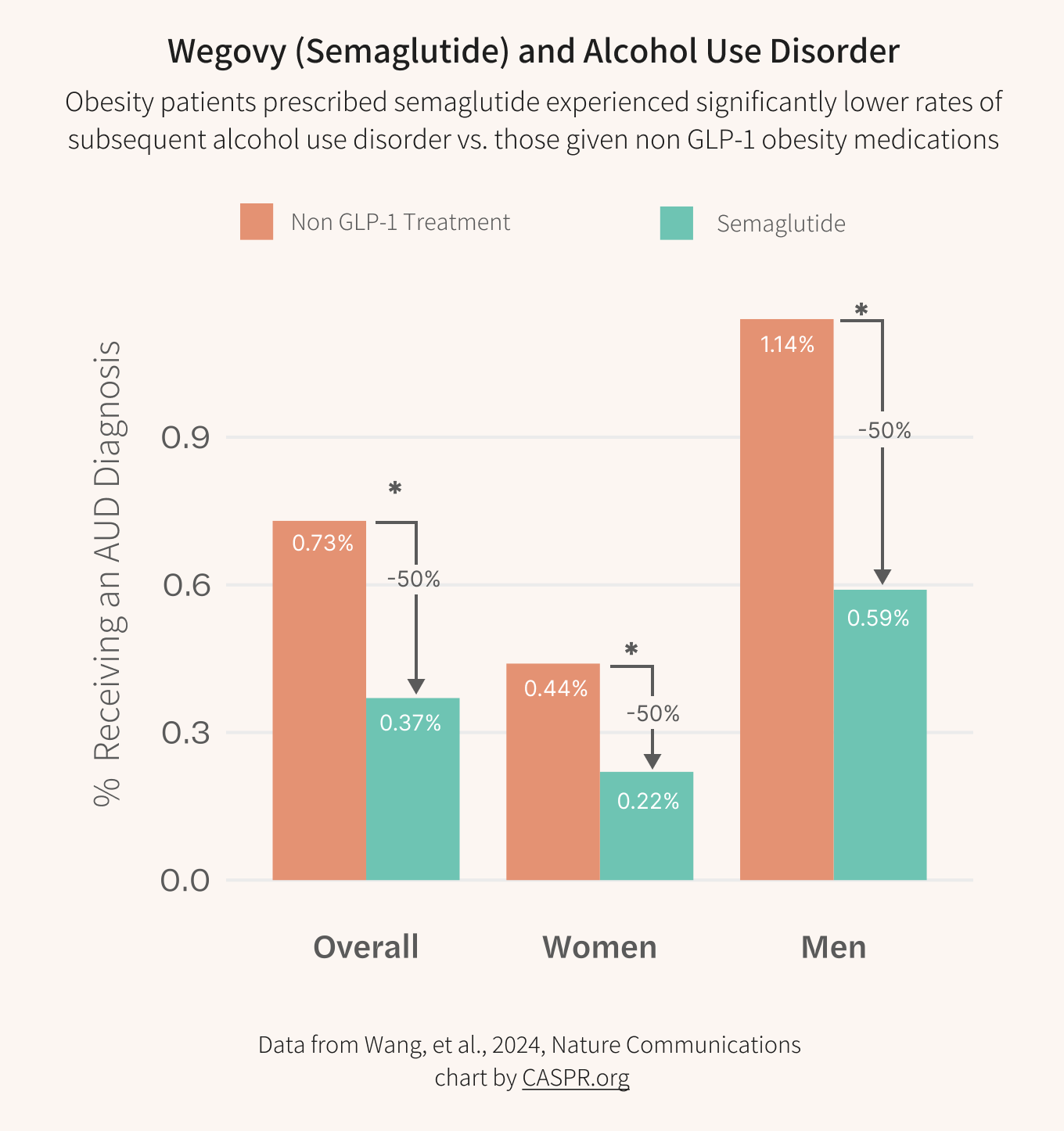
While GLP-1 was initially developed as a treatment for weight loss and diabetes, researchers are now exploring its potential in addressing a range of addictive behaviors, including substance use disorders, compulsive behaviors, and even mental health challenges. The evidence suggests that GLP-1 may be a game-changer in the treatment of addiction, offering a new dimension of care beyond traditional therapies.
Key Takeaways on GLP-1 and Food Addiction Therapy

- GLP-1 medications slow gastric emptying, increasing satiety and reducing hunger and food cravings.
- GLP-1 has been shown to reduce the severity of food addiction in clinical studies.
- The hormone regulates dopamine signaling in the brain, which plays a critical role in both addiction and obesity.
- Combining GLP-1 therapy with lifestyle changes may lead to lasting success in treating food addiction.
While the research on GLP-1 and food addiction is promising, it's essential to note that these medications are not a cure for food addiction. In many cases, individuals may experience a temporary reduction in cravings, but relapse can occur if the underlying issues are not addressed. To unlock the full potential of GLP-1 in food addiction therapy, a comprehensive approach that incorporates medication, lifestyle changes, and emotional support may be necessary.
Conclusion: The Bright Future of GLP-1 in Food Addiction Therapy
As researchers continue to explore the role of GLP-1 in addressing addictive behaviors, we may be on the cusp of a groundbreaking discovery. By targeting the brain's reward system and regulating dopamine signaling, GLP-1 may offer a new hope for individuals struggling with food addiction. While the journey ahead is still unfolding, one thing is clear: GLP-1 is a promising player in the fight against food addiction, and its potential is worth exploring further.

Moving forward, it's essential to keep these visual contexts in mind when discussing Food Addiction Therapy Glp-1.
1. Dimitri et al. (2025). Exploring the Potential of GLP-1 in Treating Food Addiction. Journal of Clinical Psychopharmacology.
2. Glucagon-like peptide-1 (GLP-1) receptor agonists: A comprehensive review. Expert Opinion on Emerging Drugs.
3. Lembke et al. (2024). GLP-1 as a potential treatment for food addiction. Journal of Addiction Medicine.
Recommended Reading:
For those interested in exploring the world of GLP-1 and food addiction therapy further, here are some recommended resources:
- Anne Lembke's article on GLP-1 and addiction in Stanford Medicine.
- The article on GLP-1 and obesity in The New York Times.
- Research on GLP-1 and substance use disorders in the Journal of Clinical Psychopharmacology.